Sunscreen works in a tanning bed. It absorbs or reflects UV radiation the same way it does outdoors, and it does reduce some of the exposure reaching your skin.
That’s the accurate answer. It’s also incomplete, because the protection you’re actually getting inside a tanning bed is significantly less than most people imagine, and the reason why matters more than the yes-or-no.
| Robin Morales is a licensed esthetician sharing professional guidance based on clinical experience. This article is educational and does not replace medical advice. For questions about UV exposure, skin cancer risk, or prescription medications, consult a board-certified dermatologist. |
The Short Answer (And Why It’s More Complicated Than Yes or No)
Sunscreen functions in a tanning bed, but the protection it offers is significantly smaller than the SPF number implies, because tanning beds emit UVA radiation predominantly, and SPF ratings measure almost exclusively UVB.
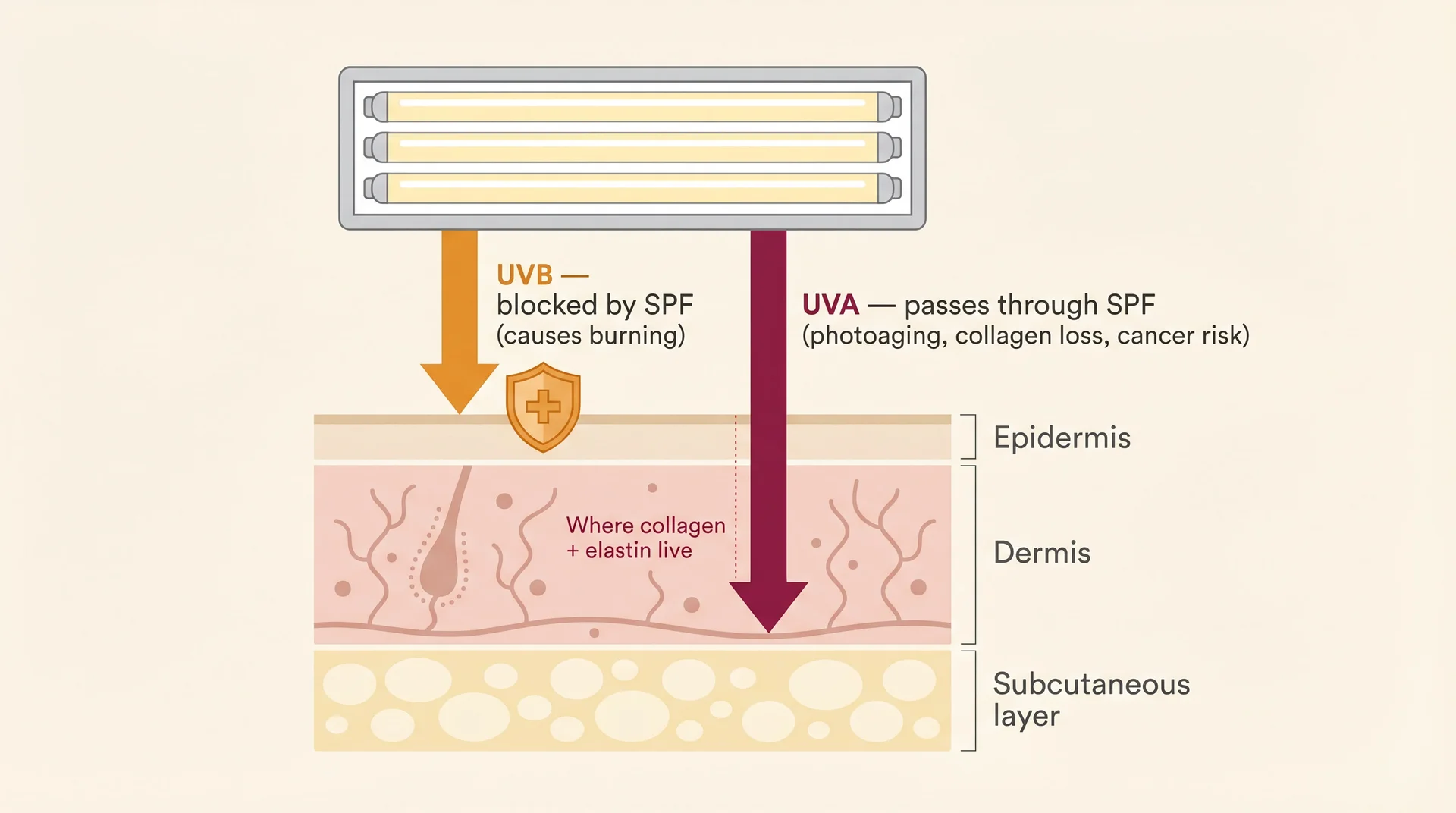
According to the MD Anderson Cancer Center, tanning beds produce about 12 times more UVA than natural sunlight. A person applying SPF 50 before a session is largely blocking the wavelength that causes burning, while the wavelength responsible for photoaging, collagen breakdown, and most skin cancer risk continues to penetrate.
This isn’t a technicality.
UVA reaches into the dermis, where it breaks down collagen and elastin and drives the kind of aging that shows up years later as thinned skin, visible capillaries, and deep wrinkling.
UVB is shorter-wavelength, causes burning, and is what SPF primarily blocks. The distinction matters because inside a tanning bed, UVA is the dominant output, and it’s the one doing the structural work.
Inside a tanning bed, the ray doing the most damage isn’t the one your sunscreen was built to stop.
What SPF Actually Measures (And What It Doesn’t)
SPF measures how much UVB radiation reaches your skin, not how much total UV protection you have. The American Academy of Dermatology is specific: SPF 15 blocks 93% of UVB rays, and SPF 30 blocks 97%.
The gap between those two numbers is smaller than most people assume, and neither figure tells you anything reliable about UVA protection. For that, you need a genuinely broad-spectrum formula, one listing zinc oxide, titanium dioxide, or avobenzone in the active ingredients.
Many standard sunscreens are not truly broad-spectrum, and even the ones that are achieve lower UVA blocking percentages than their SPF number implies about UVB.
The practical friction: most people choose sunscreen by the SPF number alone. Inside a tanning bed, where UVA dominates, chasing a higher SPF is a partial solution aimed at the wrong problem.
How Tanning Bed UV Differs From Outdoor Sun
Tanning beds do not simply replicate the sun in a smaller, more controlled space. Outdoors, UV radiation hits your skin at an angle, passes through the atmosphere, and varies with time of day and cloud cover.
Inside a tanning bed, you’re surrounded by fluorescent bulbs at close range, exposure arrives from above and below simultaneously, and the session is engineered to produce melanin response in minutes.
The FDA requires warning labels on all tanning equipment specifically because the radiation output is not equivalent to casual outdoor sun exposure. Any sunscreen you apply was formulated and tested for outdoor conditions.
How it performs under the sustained, close-range, UVA-heavy output of a tanning bed is a different question the label doesn’t answer.
You can still develop a tan while wearing sunscreen in a tanning bed, because no sunscreen blocks 100% of UV. That’s not reassurance. It means enough UV is reaching your skin to trigger melanin production, which is your body’s response to cellular damage.
Why Sunscreen on Your Face in a Tanning Bed Doesn’t Work the Way You Think
Tanning beds emit UVA radiation predominantly, and standard SPF ratings measure UVB protection, so a high SPF applied to the face still allows the dominant wavelength to reach the skin.
Applying sunscreen only to the face while leaving the rest of the body bare is probably the most common protective strategy among regular tanning bed users, and it’s also the most frequently misunderstood.
A genuinely broad-spectrum formula does provide partial protection against photoaging and pigmentation changes on the face. But it introduces a specific, unintended consequence: because the face feels covered, people tend to stay in longer or go more frequently, reasoning that the session is otherwise controlled.
Longer sessions mean more cumulative UVA exposure to the neck, chest, hands, and décolletage, all areas that age visibly and that clients often overlook until the damage has been accumulating for years.
I see the downstream effects of this pattern on clients regularly. The face holds up somewhat better than their tanning history would predict, but the chest and neck show the whole story: early wrinkling, visible capillaries, and pigmentation changes that make the overall appearance older than the face alone suggests. The skin doesn’t lie about what it’s been through.
One distinction worth clarifying here: indoor tanning lotions are an entirely different category from sunscreen. They’re designed to enhance melanin production, moisturize during a session, and optimize tanning results.
They contain no SPF and offer no UV protection whatsoever. A lot of people hold them in the same mental category as “something protective I put on before tanning.” They’re not.
Broad-Spectrum vs. SPF-Only: Which One Actually Matters Here
Inside a tanning bed, a broad-spectrum sunscreen with UVA-blocking active ingredients is the only type worth applying to the face. An SPF 50 product without genuine broad-spectrum coverage offers very limited protection against the dominant wavelength in the bed. Check the active ingredients, not the SPF number.
Zinc oxide and titanium dioxide are mineral filters that block a wider range of UV wavelengths across both UVA and UVB. Avobenzone is a chemical filter with meaningful UVA coverage. Without at least one of those on the label, the product is primarily protecting you from burning. In a timed, moderate session, burning may not be your main risk anyway.
Mineral vs. Chemical Sunscreen in a Tanning Bed Environment
Mineral sunscreens behave differently from chemical ones under tanning bed conditions, and the difference is relevant for anyone with acne-prone or sensitized skin. Chemical filters like oxybenzone and octinoxate work by absorbing UV energy and converting it to heat.
Inside a warm, enclosed bed with sustained UV output, that heat conversion happens under conditions the formulas weren’t designed for. They don’t stop working, but the process can increase the likelihood of irritation and breakouts on reactive skin.
Mineral sunscreens sit on the surface and physically deflect UV rather than absorbing it, making them the more appropriate choice if you’re going to apply anything before a session.
The practical catch is coverage. Mineral formulas, particularly at higher zinc concentrations, leave a white cast and don’t spread easily in a warm environment. Uneven application means uneven protection and an uneven tan.
Are You on Retinoids, Acne Medications, or Actives?
Tanning beds expose skin to concentrated UVA radiation, and certain skincare ingredients amplify the damage UV causes at the cellular level.
If you’re currently using tretinoin, retinol, AHAs, benzoyl peroxide, topical antibiotics, or any prescription acne treatment, your risk inside a tanning bed is meaningfully higher than it is for someone with untreated skin, and most salon staff are not going to ask you about this before you get in.
This is the section of the conversation that almost never comes up at the salon, and it’s the angle I return to most often when clients are combining an active skincare routine with regular tanning.
Retinoids work by accelerating cell turnover and thinning the stratum corneum, the outermost layer of skin that serves as the first physical barrier against UV radiation.
A skin barrier in active tretinoin use is thinner, more permeable, and more reactive to UV-induced oxidative stress than untreated skin.
The same session length that a long-time tanner handles without incident can produce inflammation, post-inflammatory hyperpigmentation, and accelerated sensitization in someone who started tretinoin six weeks ago
. The tan develops the same way on the surface. The damage underneath doesn’t.
Ingredients That Make Tanning Bed Exposure Significantly More Damaging
Several common skincare actives increase photosensitivity in ways directly relevant to concentrated UV exposure:
- Tretinoin and prescription retinoids thin the skin barrier and increase UV penetration into the dermis
- AHAs (glycolic acid, lactic acid) remove the outermost layer of dead skin cells, leaving fresh, less-protected skin directly exposed
- Benzoyl peroxide is a photosensitizer that generates reactive oxygen species more readily under UV exposure
- Oral and topical antibiotics, including doxycycline and clindamycin, carry photosensitivity warnings for outdoor sun; tanning bed UV is not a safer environment
- Salicylic acid at moderate to higher concentrations exfoliates enough to increase UV vulnerability at the surface
The pattern I see most often: someone starts a new skincare routine because they care about their skin, and they don’t connect it to the tanning sessions they’ve had for years. The tretinoin their dermatologist prescribed and the salon membership feel like separate parts of their life. At the skin barrier level, they’re not.
If you use semi-permanent brow treatments like nano brows or microblading, many of these same active ingredients also speed up pigment fading, particularly when combined with UV exposure. Our guide to nano brows vs. powder brows covers which skincare habits affect your results most.
What to Tell Your Esthetician (Or Yourself) Before a Session
Anyone using prescription or active skincare should stop retinoids at least two to three days before a session as a precautionary measure, skip AHA exfoliation for several days prior, and use only a mineral broad-spectrum sunscreen on the face during the session.
Framed as clinical guidance: that’s a reasonable minimum, not a guarantee. It reduces one part of the risk on one part of the body.
One thing that rarely comes up without prompting: eye protection. UV exposure from tanning beds reaches the eyes and can cause cataracts and other cumulative damage.
Protective eyewear designed specifically for tanning bed use is not optional, and neither closing your eyes nor wearing regular sunglasses provides adequate protection. It’s the kind of thing no one mentions until you ask.
Does Sunscreen Reduce Skin Cancer Risk in a Tanning Bed?
Sunscreen reduces but does not eliminate skin cancer risk from tanning beds, and the reduction is smaller than most people expect, because the carcinogenic exposure is predominantly UVA, and most sunscreens only partially address it.
The American Academy of Dermatology’s indoor tanning data is direct: indoor tanning increases the risk of squamous cell carcinoma by 58% and basal cell carcinoma by 24%. Using tanning beds before age 20 increases melanoma risk by 47%, and that risk rises with each additional session.
The World Health Organization and the International Agency for Research on Cancer classified UV-emitting tanning devices as Group 1 carcinogens in 2009, the same category as tobacco smoke. Sunscreen applied before a session doesn’t reclassify the device or the exposure. It modestly reduces some of the UV reaching your skin, and that’s the full extent of what it does.
What the Research Actually Says About Sunscreen and Indoor Tanning Risk
There is no research showing that sunscreen use converts indoor tanning into a low-risk activity. A December 2025 study on the molecular effects of indoor tanning, published through the Skin Cancer Foundation, found that people who use tanning beds carry more DNA damage in their skin cells than people twice their age who have never used them.
UV-induced DNA damage from each session accumulates over time. Sunscreen at typical application levels delays some of it. It does not prevent it from occurring, and the underlying risk profile of the exposure doesn’t change because you applied a product beforehand.
The False Security Problem: Why SPF Can Make Things Worse
Wearing sunscreen in a tanning bed can, counterintuitively, lead to higher cumulative UV exposure over time.
When people apply SPF before a session, they often stay in longer or go more frequently, reasoning that the protection offsets the added time. SPF also reduces burning, and burning is the primary signal most people use to gauge whether they’ve had too much.
Remove that signal, and it becomes easier to underestimate how much UV exposure is accumulating across weeks and months. The protection reduces one risk. The behavioral response to feeling protected can quietly increase another.
What Actually Happens to Your Skin Barrier During Repeated Tanning Bed Use
Tanning beds emit UV radiation that reaches deeper into the skin than most people realize, and the effects accumulate even when no burn occurs. Repeated tanning bed sessions progressively degrade the skin barrier, even with short, moderate sessions and consistent moisturizing afterward.
UVA penetrates into the dermis, where it disrupts fibroblasts, the cells responsible for producing collagen and elastin. The structural proteins weaken over time, the barrier holds moisture less effectively, and skin becomes less resilient to everyday irritants and environmental stress.
There’s no visible signal when this is happening. It builds across months and years, and by the time it shows up on the surface, the underlying structural loss is already established.
The acne connection deserves a specific explanation because it generates genuinely conflicting experiences, and the standard article either ignores it or oversimplifies.
The Sebum Rebound Cycle Explained
Tanning beds appear to clear acne because UV light initially suppresses surface bacteria and dries out excess sebum, but this effect is temporary, and the skin’s compensatory response is what drives the rebound.
The skin interprets UV-induced drying as lost lipid barrier integrity and responds by increasing sebum production. UV exposure also disrupts regular keratinocyte shedding, meaning dead skin cells are more likely to stay in the follicle and contribute to clogged pores.
In the weeks after stopping tanning, elevated sebum production and irregular cell turnover create exactly the conditions for a significant breakout.
This is why the pattern on acne forums is contradictory: tanning seems to help, stopping causes a flare, so people go back. The cycle reinforces itself, and the barrier function keeps declining with each round.
There’s a second piece most of those conversations miss: UV exposure darkens post-inflammatory hyperpigmentation, the brown or red marks acne leaves behind.
The marks look less obvious on tanned skin because the surrounding tone has shifted toward them. The pigment is still being stimulated, and it resurfaces more visibly when the tan eventually fades.
Why Tanning Bed Regulars Often Have a Compromised Skin Barrier Without Realizing It
The early signs of UV-related barrier compromise are easy to misread as something else entirely. Skin that feels tight after a session can feel like it’s been deep-cleaned. Skin that looks smoother immediately after can look refreshed and pore-refined.
Both are signs of dehydration and surface protein disruption. Over time, the same people develop increased sensitivity to products they’d used for years without issue, unexplained breakouts in new locations, and faster onset of fine lines around the eyes and corners of the mouth.
The connecting thread in clients I see with this pattern is years of indoor tanning that felt controlled, moderate, and uneventful at the time.
Rebuilding a depleted skin barrier requires consistent support with ingredients like ceramides, fatty acids, and humectants.
If the patterns above sound familiar, you should read this blog on Korean milky toners, which covers how barrier-focused layering works and what to look for in formulas designed for compromised or sensitized skin.
Safer Alternatives That Actually Give You the Results You’re After

Self-tanners are genuinely worth reconsidering if your frame of reference is a product from a decade or more ago. Modern formulas have changed. The orange undertone problem that defined early DHA-based products has largely been resolved by formulations that blend DHA with erythrulose and include tinted guide color to prevent missed patches.
There are options now that build natural-looking color on a range of skin tones, dry down without transferring to fabric, and hold for several days with proper prep.
The specific challenge for acne-prone or sensitive skin is finding something that doesn’t congest pores or trigger a reaction. Most full-coverage body self-tanners are too occlusive for the face.
This is where a lot of people have a bad first experience and write off the whole category. The problem is usually the formula, not the concept.
Self-Tanners That Work for Acne-Prone and Sensitive Skin
Fragrance-free, non-comedogenic, water-based formulas are the starting point for acne-prone skin. For anyone who has broken out from self-tanners previously, the issue is almost always the base, not the DHA itself.
Many formulas use heavy emollients that sit in pores, particularly on the face and chest. Gradual formulas allow the skin to adjust and make early sensitivity easier to catch before you’ve applied a full treatment.
For body use, applying over freshly exfoliated, completely dry skin and waiting at least 20 minutes before dressing produces the most even result. For the face, a low-concentration gradual formula used as a daily moisturizer builds color slowly enough that it rarely looks artificial and gives you an early exit if anything reacts.
How to Maintain a Natural-Looking Base Without UV Exposure
A bronzing powder or tinted moisturizer gives immediate, adjustable color with no UV exposure and no commitment.
For a longer-lasting base, a gradual self-tanner applied to the legs and arms two to three times a week maintains consistent color that holds through normal activity.
Keeping skin well-hydrated between applications is practical, not just a skincare nicety: dry skin sheds faster, and self-tanner color fades unevenly when it does.
Final Thoughts
The question of whether sunscreen works in a tanning bed has a genuine answer: yes, it functions, and a broad-spectrum formula is better than nothing.
But the SPF number overstates what you’re actually getting, the UVA doing most of the long-term damage is only partially addressed even by the best formulation, and if your routine includes retinoids or actives, the risk before a session is higher than most people realize.
For anyone looking to keep the results while reducing what it costs their skin, that information is the actual starting point.








